What is Mean Arterial Pressure (MAP)?
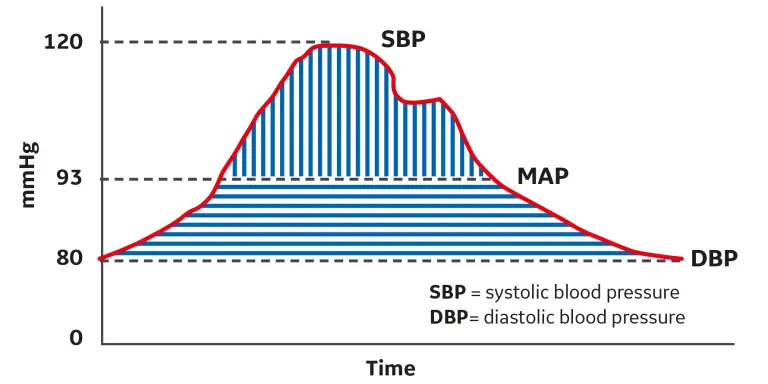
MAP is the average pressure in your arteries during one complete heartbeat (one full cardiac cycle).
Here's the thing most people don't realize: your heart doesn't pump at a steady pressure. It squeezes (systole), then relaxes (diastole). The pressure goes up, then down. Over and over.
MAP captures what the average pressure actually is throughout that whole cycle. And that average? It's a better indicator of tissue perfusion than either systolic or diastolic pressure alone. Way better.
Why is MAP Important?
Your organs need consistent blood flow. Brain. Heart. Kidneys. They don't care about your peak pressure. They care about the average.
When MAP drops below 60 mmHg, you're in trouble. Organs start getting damaged because they're not getting enough perfusion. Tissue starts dying.
This is why ICU monitors track MAP, not just regular blood pressure.
Surgeons watch it during operations. Critical care teams watch it constantly. If you have hypertension or hypotension, your doctor is probably calculating your MAP even if they don't tell you about it.
It's one of those numbers that matters more than people think.
How to Use the MAP Calculator
Pretty straightforward.
- Enter your systolic blood pressure in mmHg (the top number)
- Enter your diastolic blood pressure in mmHg (the bottom number)
- The calculator does the math instantly
That's it. Takes two seconds.
Some calculators let you toggle between different formula versions. Both give you the same answer mathematically, so don't overthink it. Just enter your numbers.
MAP Formula: How to Calculate Mean Arterial Pressure
There's a reason the formula looks the way it does. And yeah, it's a little weird at first glance.
The standard MAP formula is:
Or you can write it this way:
Same thing. Different arrangement.
DBP is diastolic blood pressure. SBP is systolic blood pressure.
Notice diastolic gets weighted more heavily. That's not random. Your heart spends about twice as long in diastole (relaxing) as it does in systole (contracting). So diastole contributes more to the average pressure. The math reflects the physiology.
Standard MAP Formula

Let's break this down.
The (SBP − DBP) part is called pulse pressure. It's the difference between the two readings. You're taking one-third of that and adding it to diastolic.
Why one-third? Because systole only accounts for about one-third of the cardiac cycle. Diastole takes the other two-thirds. Roughly speaking.
Example calculation (blood pressure: 120/80 mmHg)
That's a healthy MAP. Right in the normal range.
Alternative MAP Formula
Same math, cleaner setup for mental calculation.
Same example (120/80 mmHg).
Identical answer. Some people find this version easier to do in their head. I do.
MAP Calculation Example
Let me run through a few scenarios so you can see how this plays out.
Example 1
Normal Blood Pressure (120/80 mmHg)
Normal range
Example 2
Hypertension (160/100 mmHg)
Elevated
Example 3
Hypotension (90/60 mmHg)
Low end of normal, borderline
See how the numbers shift? The hypotensive patient is right on the edge. A little lower and you're looking at perfusion problems.
Normal MAP Range: What's Healthy?
70–100 mmHg. That's the target.
Optimal sits around 90 mmHg, give or take.
Below 60 mmHg is the danger zone. That's the minimum threshold for adequate organ perfusion. Below that, your kidneys, brain, and heart aren't getting what they need.
Now, there's some individual variation. Age matters. Activity level matters. Some people run a little higher or lower and they're fine. But as a general rule, you want to be somewhere in that 70–100 range.
What Does Low MAP Mean? (Hypotension)
Low MAP means your blood isn't pushing hard enough. Generally, we're talking about MAP below 60–65 mmHg.
What causes it
- Severe blood loss
- Heart failure
- Sepsis
- Dehydration
- Medication side effects (blood pressure meds, sometimes others)
What it feels like
- Dizziness
- Fainting or near-fainting
- Fatigue that won't quit
- Blurred vision
- Nausea
Why it's dangerous
Organs stop getting enough blood. Tissues start dying. You can go into shock. This isn't something to mess around with.
If you're symptomatic and your blood pressure is dropping, get medical help. Especially if it's sudden.
What Does High MAP Mean? (Hypertension)
High MAP means consistently above 100 mmHg. Usually indicates chronic hypertension.
What causes it
- Chronic high blood pressure
- Kidney disease
- Endocrine problems
- Chronic stress
- Obesity
The tricky part
It's often silent. No symptoms. People walk around with elevated MAP for years without knowing.
When symptoms do show up, you might get headaches. Shortness of breath. Occasional nosebleeds. But a lot of people feel nothing until something bad happens.
Long-term risks
- Stroke
- Heart attack
- Kidney failure
- Aneurysm
This is why regular checkups matter. You can't feel high MAP, but it's doing damage.
Factors Affecting Mean Arterial Pressure
MAP isn't static. It changes based on what's happening in your body.
Four main players: cardiac output, systemic vascular resistance, blood volume, and how elastic your blood vessels are. Let's go through them.
1. Cardiac Output
Cardiac output = heart rate × stroke volume. Basically, how much blood your heart pumps per minute.
More cardiac output, higher MAP. Simple relationship.
Exercise increases cardiac output temporarily. So does stress, caffeine, certain medications. Heart conditions can decrease it.
Your heart pumping stronger and faster means more pressure in the arteries.
2. Systemic Vascular Resistance (SVR)
This one's about how much resistance blood encounters as it moves through your vessels.
- Vasoconstriction (vessels tightening) increases SVR. MAP goes up.
- Vasodilation (vessels relaxing) decreases SVR. MAP goes down.
What affects SVR? Vessel diameter is the big one. Blood viscosity matters too — thicker blood, more resistance. Even vessel length plays a role, though that's pretty fixed.
Cold weather causes vasoconstriction. That's one reason blood pressure tends to run higher in winter.
3. Blood Volume
More fluid in the system, higher the pressure. Like turning up the water pressure in a hose.
Things that affect blood volume
- Hydration status (dehydrated = lower blood volume)
- Blood loss
- Kidney function (kidneys regulate fluid balance)
- Hormones like aldosterone and ADH
This is why people with chronic kidney disease often have blood pressure issues. Their kidneys can't regulate fluid properly.
4. Vessel Elasticity
Healthy arteries are flexible. They expand a little when blood pushes against them, then recoil back. That absorbs some of the pressure.
Stiff arteries don't do that. Blood slams against rigid walls. Pressure stays elevated.
Atherosclerosis hardens arteries. So does age. Diabetes. Chronic hypertension itself makes vessels stiffer over time.
It becomes a vicious cycle. High MAP damages vessels. Damaged vessels become stiffer. Stiff vessels increase MAP further.
5. Age and Gender
MAP generally increases as you get older. Vessels get stiffer. Kidneys work a little less efficiently. Normal aging stuff.
Gender differences exist too, though they're complicated. Hormones play a role — estrogen has some protective effects on blood vessels, which is why women's cardiovascular risk changes after menopause.
Lifestyle factors interact with all of this. Someone who's active and eats well at 60 might have better MAP than a sedentary 35-year-old.
When Should You Check Your MAP?
Not everyone needs to calculate their MAP constantly. But some situations call for it.
You should think about MAP if you have:
- Chronic hypertension
- Pre-existing cardiovascular disease
- Pregnancy (preeclampsia is a real concern)
- Recent surgery
- Symptoms of blood pressure problems
Regular checkups catch most issues. But if you're in one of these categories, it's worth understanding what your MAP actually is, not just your blood pressure reading.
MAP During Pregnancy
Pregnancy changes everything about blood pressure. Blood volume increases dramatically. Cardiac output goes up. Hormones shift.
MAP monitoring helps catch preeclampsia early. That's a serious pregnancy complication involving high blood pressure and organ damage. It can develop quickly.
Normal pregnancy does cause some blood pressure changes. It typically drops a bit in the second trimester, then rises again in the third. But a significantly elevated MAP, especially with other symptoms like protein in urine or swelling, is a red flag.
Regular prenatal care catches this. Don't skip appointments.
Common Questions
What is a dangerous MAP level?
Below 60 mmHg is critical. Organs aren't getting adequate perfusion. This is emergency territory.
Above 110–120 mmHg chronically significantly increases risk for cardiovascular events. Stroke. Heart attack. Aneurysm rupture.
Acute vs. chronic matters here. A brief spike during exercise or stress isn't the same as sustained elevation. Your body can handle temporary increases. It's the chronic high levels that cause cumulative damage.
If MAP drops suddenly and you're feeling symptoms (dizziness, confusion, rapid heartbeat), seek emergency care. If it's chronically elevated and you're not being treated, you need to see a doctor.
Is MAP the same as blood pressure?
No. Different things.
Blood pressure gives you two numbers: systolic over diastolic. That's the peak pressure and the minimum pressure.
MAP is the calculated average across the whole cardiac cycle. It accounts for the fact that your heart spends different amounts of time in systole versus diastole.
Think of it this way. Blood pressure reading tells you the range. MAP tells you the average. Both matter, but they're measuring different aspects of the same phenomenon.
What MAP is needed for brain perfusion?
The brain is picky about blood flow. It needs consistent supply.
Generally, a MAP of 60 mmHg minimum is required for adequate cerebral perfusion. But there's a buffer.
The brain has autoregulation. Between MAP of about 60–150 mmHg, it adjusts its own vascular resistance to maintain stable blood flow. Below 60, that autoregulation fails. Above 150, it also fails in the other direction.
This is why these ranges matter so much in neurocritical care. Stroke patients. Traumatic brain injury. Neurosurgery. Keeping MAP in the right zone is literally the difference between brain damage and recovery.
How often should MAP be monitored?
Depends entirely on the situation.
- Healthy individuals: During routine checkups. Maybe once or twice a year. Your doctor calculates it from your regular blood pressure reading anyway, even if they don't mention it.
- Chronic hypertension patients: As often as your doctor recommends. Might be monthly, might be more frequent during medication adjustments.
- Critically ill patients: Continuously. ICU monitors track MAP in real-time.
- Post-surgical patients: Per protocol, usually multiple times daily until stable.
If you're healthy and don't have risk factors, don't obsess over it. If you have cardiovascular issues, talk to your doctor about what makes sense for your situation.
Does MAP change with body position?
Yes. Gravity affects blood pressure.
When you stand up from lying down, MAP typically decreases slightly. Your body compensates by constricting blood vessels and increasing heart rate. Usually you don't notice.
But some people have orthostatic hypotension. Their MAP drops significantly when they stand. They get dizzy. Sometimes they faint.
This is why proper measurement technique matters. Blood pressure should be measured consistently — same position each time, ideally after sitting quietly for a few minutes. Standing measurements tell you something different than sitting measurements.
If you feel lightheaded every time you stand up, mention it to your doctor. It can indicate underlying issues with blood pressure regulation.